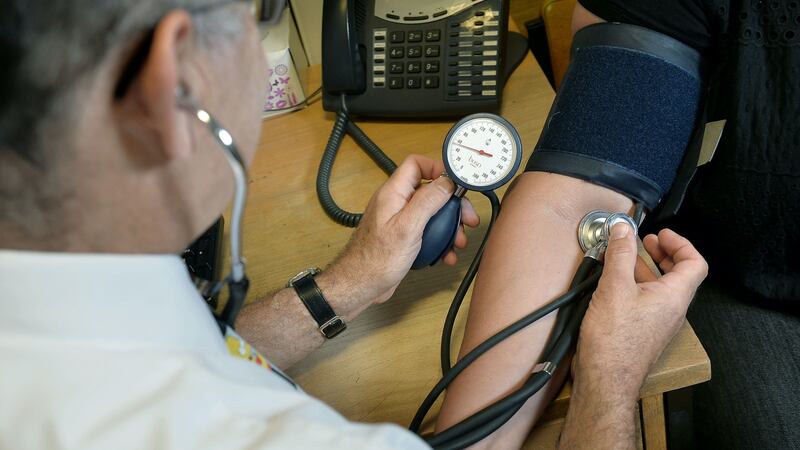
Higher than normal blood pressure in midlife may be linked to more extensive brain damage in the elderly, new research suggests.
The new study indicates there is a strong association between diastolic blood pressure (the blood pressure between heartbeats) before the age of 50 and brain damage in later life.
According to the research, this also applied if the diastolic blood pressure was within what is normally considered to be a healthy range.
The findings come from a study of 37,041 participants enrolled in UK Biobank, a large group of people recruited from the general population aged between 40 and 69 years.
Dr Karolina Wartolowska, a clinical research fellow at the University of Oxford, looked for damage in the brain called white matter hyperintensities (WMH).
These hyperintensities show up on MRI brain scans as brighter regions and indicate damage to the brain’s small blood vessels. This damage increases with age and blood pressure.
WMH are associated with an increased risk of stroke, dementia, physical disabilities, depression and a decline in thinking abilities.
Dr Wartolowska said: “Not all people develop these changes as they age but they are present in more than 50% of patients over the age of 65 and most people over the age of 80 even without high blood pressure.
“But it is more likely to develop with higher blood pressure and more likely to become severe.”
Systolic blood pressure is the maximum blood pressure reached each time the heart beats and is the top number in blood pressure measurements.
The study, published in the European Heart Journal, found that a higher load of WMH was strongly associated with current systolic blood pressure.
The strongest association was for past diastolic blood pressure, particularly when under the age of 50, researchers found.
For every 10mmHg (millimetres of mercury) increase in systolic blood pressure above the normal range, the proportion of WMH load increased by an average of 1.126-fold, and by 1.106-fold for every five mmHg increase in diastolic blood pressure.
Among the top 10% of people with the greatest WMH load, 24% of the load could be attributed to having a systolic blood pressure above 120mmHg.
Dr Wartolowska said: “We made two important findings.
“Firstly, the study showed that diastolic blood pressure in people in their 40s and 50s is associated with more extensive brain damage years later.
“This means that it is not just the systolic blood pressure, the first, higher number, but the diastolic blood pressure, the second, lower number, that is important to prevent brain tissue damage.
”The second important finding is that any increase in blood pressure beyond the normal range is associated with a higher amount of white matter hyperintensities.
“This suggests that even slightly elevated blood pressure before it meets the criteria for treating hypertension has a damaging effect on brain tissue.”
Potential mechanisms for the development of WMH include damage to the delicate blood vessels in the brain through sustained elevated pressures, this leads to the lining of the vessels becoming leaky and results in WMH.
Alternatively, diastolic pressure might cause large blood vessels to become stiffer with time which increases pulsations of blood pressure to the brain.
As MRI scans were only available at one time point, the researchers could not quantify the progression of WMH directly.
Further analysis is also needed to identify differences in different regions of white matter.