Machine-learning has been used to develop a pioneering test which accurately predicted potential premature births in almost three-quarters of women with an asymptomatic high risk.
Researchers at the University of Warwick “trained” a device to look for chemical vapour patterns associated with pre-term birth, using vaginal swabs taken during routine examinations.
After analysing swabs from 216 asymptomatic women, it forecast an outcome of premature delivery in 73% of cases, set out in findings published in Scientific Reports.
It is hoped the technology could lead to a cost-effective, non-invasive, point-of-care test for women identified as at risk of premature delivery, and consequently reduce risks to both mother and baby.
Pre-term birth is the leading cause of death in children under five and there are few accurate tools to predict who is going to have a premature baby.
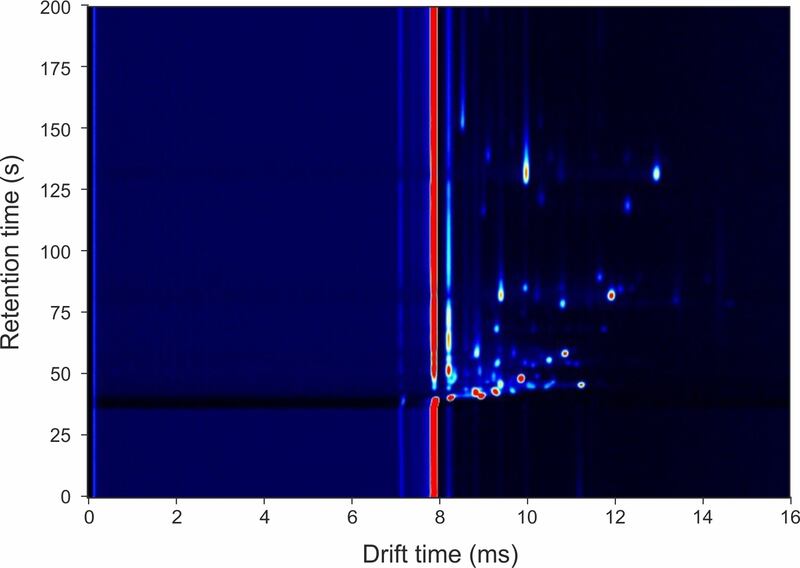
The technology focused on analysis of volatile organic compounds (VOCs) present in the vagina for a condition called bacterial vaginosis.
Previous studies have showed presence of the condition is associated with increased risk of premature births.
Researchers then “trained” the technology to spot patterns of VOCs which were signs of bacterial vagninosis.
The team then analysed swabs from women attending a specialist clinic, who had either a history of pre-term birth or a medical condition that increases the risk of such an outcome.
Analysis of swabs from the second trimester, compared against the eventual outcome of the birth, showed the technology was accurate in 66% of cases.
Scrutiny of swabs taken in the third trimester had 73% accuracy.
The results meant seven out of 10 women with a positive test went on to deliver pre-term.
Nine out of 10 women with a negative test delivered after 37 weeks, which is considered full-term.
Lead author Dr Lauren Lacey, of Warwick Medical School, is an obstetrics and gynaecology registrar at University Hospitals Coventry and Warwickshire NHS Trust (UHCW).
She said: “We’ve demonstrated the technology has good diagnostic accuracy, and in the future it could form part of a care pathway to determine who would deliver pre-term.
“Although the first test taken earlier in pregnancy is diagnostically less accurate, it could allow interventions to be put in place to reduce the risk of pre-term delivery.
“For the test towards the end of pregnancy, high-risk women can have interventions put in place to optimise the outcome for baby.
“There are a number of different factors that could cause a woman to go into pre-term labour.
“Because of that, prediction is quite difficult.
“There are lots of things we can look at – the patient’s history, the examination, ultrasound scan, various other biomarkers that are used in clinical practice.
“No single test fits all.”
She added: “VOC technology is really interesting because it reflects both the microbiome and the host response, whereas other technologies look for a specific biomarker.
“It’s the beginning of looking at the association of VOCs with pre-term delivery.
“We want to develop this and look at whether these patterns could be implemented into a care pathway.”
The next stage of research would see a small VOC analysis device stored at a hospital so samples could be analysed on site.
It is hoped the tool could eventually be developed for use in labour-ward triage, allowing rapid turnaround on test results.
Professor James Covington, from the University of Warwick School of Engineering, said he believed the technology behind the test would “become commonplace” in the identification of many diseases in the near future.
“There is a strong interest around the world in the use of vapours emanating from biological waste for the diagnosis and monitoring of disease,” he said.
“These approaches can non-invasively measure the health of a person, detect an infection or warn of an impending medical need.”
He added: “For the need described in the paper, the technology can be miniaturised and easily located in a maternity ward.
“The analysis only takes a few minutes, the instrument needs no specialised services – just power – and is easy to use.”
The researchers behind the study are part of the newly-established Centre for Early Life, based at the university’s Medical School.
The centre builds on the university’s expertise in early life research and is aiming to pioneer research in the field.