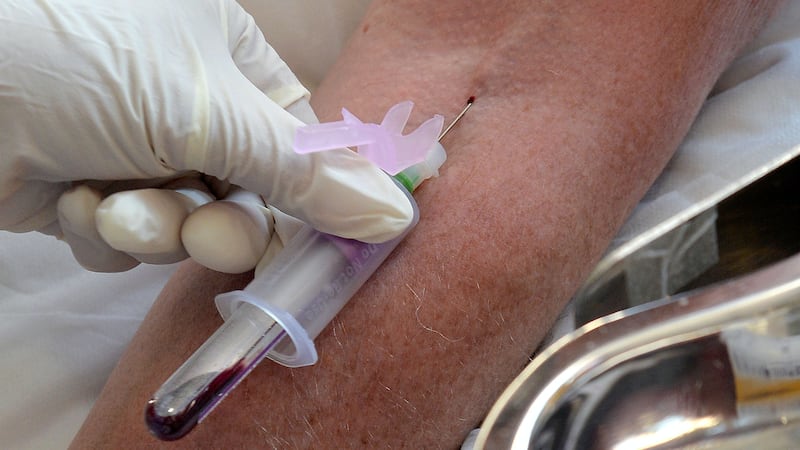
A blood test that can identify a variety of mutations in advanced breast cancer can reliably match women to effective targeted treatments, early results of a clinical trial suggest.
Experts say the plasmaMATCH trial provides the strongest evidence yet that simple blood tests known as “liquid biopsies” can benefit women with breast cancer.
They do this by tracking their disease as it evolves and directing them to the most effective treatments.
Researchers found the blood test is now reliable enough to be offered to patients on the NHS once it has passed approval, potentially raising the prospect of a major reshaping of care that could speed up access to the best available drugs.
A team at the Institute of Cancer Research, London (ICR), and The Royal Marsden NHS Foundation Trust analysed blood samples from more than 1,000 women with breast cancer that had recurred after treatment or spread to another part of the body.
They analysed whether the blood test could help improve treatment for the significant proportion of women whose breast cancer is caused by one of a variety of rarer mutations – as opposed to better-known defects like BRCA mutations.
According to the study published in Lancet Oncology, the scientists were able to reliably detect mutations found in tumour DNA that had been shed into the bloodstream of women with advanced breast cancer.
Patients were then matched to targeted treatments according to the specific mutations in the tumour DNA.
Study leader Nick Turner, professor of molecular oncology at the ICR and head of the Ralph Lauren Centre for Breast Cancer Research at The Royal Marsden, said: “Our findings show that simple blood tests can quickly and accurately tell us the genetic changes present in a patient’s cancer, and use that information to select the most suitable available treatment.
“Using a liquid biopsy could be particularly important for patients with advanced breast cancer, to help select the most appropriate treatment.
“Tests that detect tumour DNA in the blood have huge potential and could transform how doctors select targeted therapies for patients with advanced cancer.
“Our study shows that these liquid biopsies can pick up the mutations that drive a patient’s breast cancer, and can successfully match patients with the best available precision medicine for their cancer.”
The researchers looked at three targetable defects in genes called HER2, AKT1 and ESR1, which are known to drive breast cancer.
A total of 142 women with these detectable mutations were then given experimental drugs targeted against the specific characteristics of their cancer.
Women with ESR1 mutations were treated with fulvestrant, while women with HER2 mutations received neratinib on its own or with fulvestrant.
Those with AKT1 mutations were split into two groups, according to whether their cancer was oestrogen receptor positive or not, and were treated with capivasertib plus fulvestrant, or with capivasertib on its own.
The researchers found some women with HER2 and AKT1 mutations responded to the treatments assigned to them.
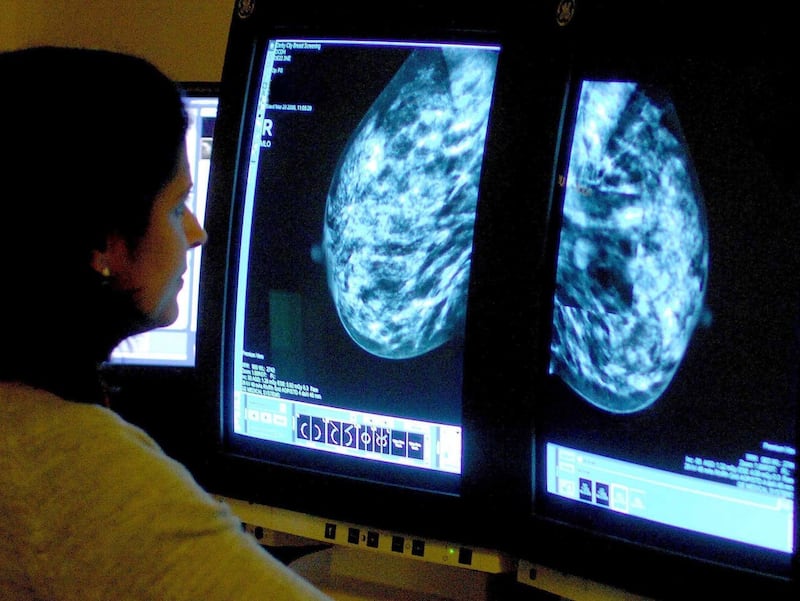
They say this indicates liquid biopsies can successfully match patients with certain rare forms of advanced breast cancer to more effective treatments.
Five out of 20 women with rare HER2 mutations who were matched to neratinib saw a beneficial response.
Four out of 18 patients with AKT1 mutations responded to capivasertib. However, the treatment targeting the ESR1 mutation was not found to be effective.
Researchers validated the findings by checking tissue samples from the patients to confirm the liquid biopsies had correctly identified the presence or absence of the mutations in over 93% of cases – sufficiently accurate to implement in routine care, they say.
For the targeted drugs that have shown promise in this study, the next step is to carry out larger clinical trials.
Dr Simon Vincent, director of research, support and influencing at the charity Breast Cancer Now, said: “This is a significant development in the field of liquid biopsies, with this blood test being shown to give some women with advanced breast cancer accurate and valuable genetic information about their disease while being less invasive than a standard biopsy.
“We look forward to seeing results from larger clinical trials and further insight into how these liquid biopsies could be used on the NHS to help select the most suitable treatment for women with advanced breast cancer.”
The plasmaMATCH trial was largely funded by Stand Up To Cancer, a joint fundraising campaign from Cancer Research UK and Channel 4, with additional support from AstraZeneca, Breast Cancer Now and Puma Biotechnology.