Q: MY HAIR has been falling out for well over a year, even though I’ve spoken to a trichologist. Two years ago I became constipated and, after trying various medications, my consultant says there is nothing more he can do. Is my hair loss caused by my poor bowel health?
PT
A: The two conditions you describe – widespread hair loss and chronic constipation – are understandably difficult to live with and, as you suggest, certainly may be linked. I suspect that link is a thyroid-related problem.
Hair loss is a common symptom that can have many causes, all of which would need to be considered before reaching a diagnosis.
These include medical treatments such as chemotherapy; poor diet; psychological stress; childbirth; and chronic iron deficiency.
As I understand it, none of the above applies in your case, hence why I turn to thyroid conditions, which are a major cause of hair loss.
The constipation – which you say has been investigated with a colonoscopy, and nothing suspicious was found – suggests you could have an underactive thyroid. This might tie together the two symptoms in an otherwise healthy individual.
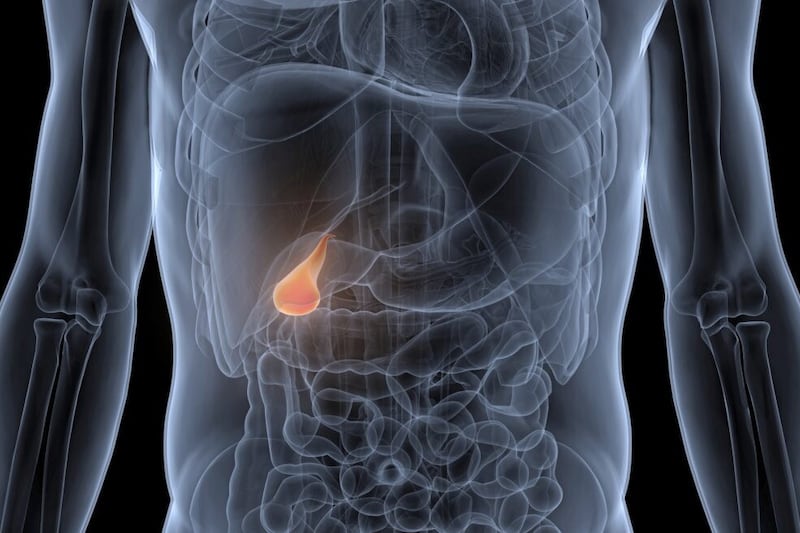
The thyroid is a butterfly-shaped gland in the front of your neck that produces hormones including thyroxine.
This controls a number of functions throughout the body, including metabolism, hair growth and digestion.
Low levels of the hormone can slow down the intestines, which can cause constipation.
An underactive thyroid is most commonly due to an autoimmune disease, where the immune system mistakenly attacks the body.
While you’ve mentioned constipation and hair loss, typically an underactive thyroid can also cause fatigue, cold intolerance and weight gain (and you do mention commencing a diet prior to the onset of the constipation).
I suggest that you ask your GP to order a blood test to check your thyroid function.
If you do have an underactive thyroid, your GP will prescribe a daily replacement dose of thyroxine, which you will take for the rest of your life. It should resolve your problems over a period of some months.
Q: FOR the past couple of years when I wake during the night, I have a burning, tingling sensation in both my lower legs. It is unpleasant and annoying. Is there anything I can do? I am 70.
DC
A: I wonder whether your sleep position lies at the root of the issue. Certainly the tingling sensations – which are presumably relieved during the daytime – seem to indicate nerve root irritation in the lower spine, which can be triggered by this.
As we age, the spinal cord (which is protected by the bony cage of the spine) can become compressed. This is because, over the years, the vertebrae naturally become worn from use – what we call osteoarthritic degeneration – causing pain and inflammation.
As part of the healing response, the body produces new spurs of bone, or osteophytes. These spurs narrow the gap in the spinal canal that carries the spinal cord (known as spinal stenosis).
Your spine and trunk muscles will also be weaker due to natural degeneration with age, and muscle strength is vital to support the spine.
The cumulative effect of this could mean that there is pressure on nerve roots, and the result is the tingling sensation you experience in your legs.
This pressure can be triggered by certain movements – possibly, in your case, when you are lying down, with the muscles of your back relaxing.
All of this is only educated guesswork, and to confirm this you will need to see your GP.
They might decide to refer you to have the nerve function in your legs checked through a nerve conduction study, carried out by a technician or a neurophysiologist in hospital.
This typically involves administering small, entirely painless electric shocks at one end of the leg, while recording the impulse at the other end using an electrode. This conveys the recorded data to an electronic ‘black box’.
We use this test in order to check for peripheral neuropathy (nerve damage).
I’d also suggest a referral for a scan of your lower back, to help identify if the pain is due to nerve pressure from spinal disease such as osteoarthritis.
If a specialist confirms that your problem is the result of spinal stenosis, you should see a rehabilitation physiotherapist.
They will offer advice and a regular training programme to improve muscle tone, and thereby increase the spine’s support system.
© Solo dmg media