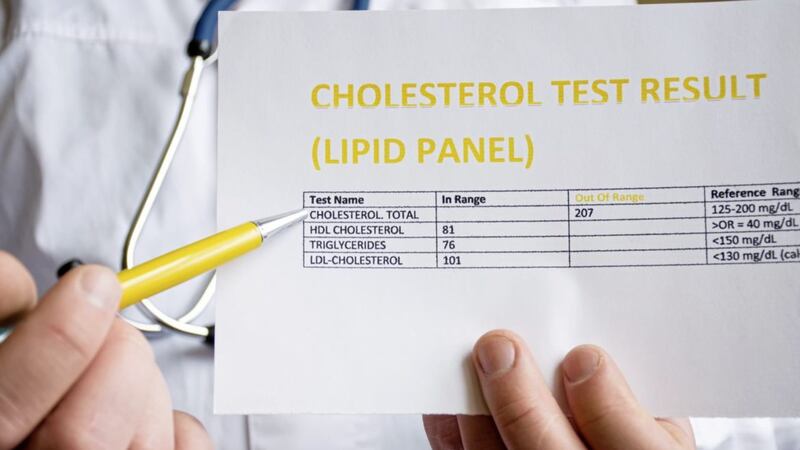
Q: I WONDER if you could explain cholesterol readings? I was told mine was 4.1 but was also given other numbers. I am 74 and healthy, but can’t take statins without awful side-effects.
LP
A: Cholesterol readings can be confusing – not least because some cholesterol is actually good for us.
We need a small amount of blood cholesterol because the body uses it to make hormones such as oestrogen and testosterone, and to help your metabolism work efficiently. But too much, and the wrong kind, can contribute to heart disease.
Cholesterol comes from two sources: our liver produces it, and we also get it from the foods we eat. It is carried in the blood in particles known as lipoproteins. The most commonly known types of cholesterol are low-density lipoprotein (LDL, or ‘bad’ cholesterol) and high-density lipoprotein (HDL, or ‘good’).
High levels of LDL are a risk factor for coronary artery disease; heart attacks; and damage to the arteries inside the brain, which can cause a stroke.
HDL, in contrast, is protective because it helps remove LDL from your bloodstream. Many people are familiar with the target level for total cholesterol being 5.0 mmol/litre. The evidence suggests that, in the long term, we are safest if our level is below this.
However, this figure includes both the damaging LDL and HDL, and the balance between the two is important.
When the figures arrive as a lab report there will be a LDL level, a HDL level, and the ratio of HDL to the total level.
As you say in your longer letter, your level of HDL is 1.7 and it is recommended that it should be below 1.2.
Your ratio, at 3.5, is also slightly high, as it ought to be below 3. This means you have more HDL than is ideal (you might think you can’t have too much of a good thing, but in fact there is an optimum level, above which it no longer confers benefit).
I note that your LDL is 3.6 and it would be preferable if it was below 3, but I wouldn’t be too concerned, as it is only minimally high. The figure of 4.1 you were given includes this and other blood fats called triglycerides.
Furthermore, a judgment about your risk of arterial disease cannot be made based on cholesterol levels alone.
Doctors agree that marginal elevations of cholesterol are not as important as other risk factors. We use a calculation called QRISK2, which factors in your age, sex, body mass index, ethnicity, family history, blood pressure, cholesterol levels and medical history.
Statins are prescribed if your score shows a greater than 20 per cent chance of developing arterial disease in the next ten years. The drugs lower the level of LDL by reducing the production of it in the liver.
As you are unable to tolerate statins because of side-effects, another option is ezetimibe, a drug that reduces the absorption of the cholesterol in your diet. I’d suggest you discuss this with your doctor when you request the result of a QRISK2 profile.
However, at 74 and with only marginal increases in your cholesterol levels, I am not convinced that drug treatment is essential in your case.
Q: I WAS diagnosed with posterior vitreous detachment which has resulted in a flashing light in my right eye. I have been informed that in rare cases, a retinal detachment may occur. Is there a procedure that could help?
MJ
A: The part of the eye behind the lens is filled with a gel called the vitreous humour. This helps the eye to maintain its shape, and it becomes more watery as we age.
The result is that it shrinks away from the retina – the light-sensitive nerve cells that line the back of the eye, which convert images into electrical impulses that are sent to the brain.
That shrinkage is called posterior vitreous detachment (PVD) and most often occurs between the ages of 50 and 75.
It may, however, happen earlier in people who are shortsighted; when there is other trauma to the eye; or after an inflammatory disorder.
If you have PVD, there is a 3.4 per cent chance that you will develop a retinal tear.
Symptoms of PVD are a sudden onset of floaters or specks in the vision. These are made up of debris in the vitreous, which are mainly collagen fibres.
There may also be a period – some days or weeks – in which sufferers experience flashes of light which last for several seconds or minutes.
Be reassured that if you have PVD but experience no retinal tear you won’t need further treatment. The floaters gradually resolve themselves, but can be bothersome for a time.
If the flashes of light worsen, immediate reassessment by an ophthalmologist is called for. But eventually the flashing light sensations will ease up.
There is a procedure – vitrectomy – in which the vitreous is removed, and this will get rid of the floaters. However, it is not appropriate for treating floaters alone, and is carried out only when repair surgery, such as retina reattachment, is needed.
© Solo dmg media