GROWING up, diabetes wasn't one of the diseases I knew about.
It wasn't in the family and I was blissfully unaware of its seriousness until I met my now husband Michael Conaghan, a mid-Ulster guy. In fact, this state of ignorance continued until 1998 when Michael, then in his early thirties, started becoming ill.
The fact that he was becoming quite poorly was disguised by the fact that I'd been hospitalised with serious food poisoning and complications, so we didn't initially notice that Michael was losing weight.
We were based in England then and I remember going to London with him pre-Christmas 1997 to meet three of his siblings for a drink and seeing their very worried faces. By now, he was pretty weak and tired as well and obviously needed to sit down in the pub while we could have happily stood at the bar and chatted. Naturally, as a concerned partner, I tried to get him to consult our GP but he was in a kind of denial. Michael was really acting out that old cliche about men avoiding medical care. He was drinking cherry colas by the bottle and his sweet tooth, normally nothing in comparison to mine, was rampant.
Honestly we should have known this was diabetes as Michael exhibited all the other classic symptoms: going to the loo several times a night, extreme thirst and weakness.
As Florence Findlay White, National Care Advisor to Diabetes UK, points out, his symptoms were fairly classic. "With type 1 diabetes the symptoms come on very quickly and we call them the four `T's. That is, going to the toilet more frequently, feeling thirsty, feeling tired and getting thinner."
For type 2, she says, add in having a dry mouth or feeling thirsty, passing more urine, especially at night and feeling physically tired. In some cases, people experience blurred vision or tingling in the feet and hands. But type 2 diabetes, the more common complaint which has led to the upsurge in numbers, may be asymptomatic.
“For reasons that are not yet understood cases of Type 1 diabetes have increased over the years, but not at the same rate as Type 2, which has risen by 60 per cent in the last decade,” said Ms Findlay White.
“The rise in Type 2 is down to a combination of factors. Some we have no control over, such as family history, ethnicity or the fact that people are living longer and reaching an age where diabetes is a higher risk. However, unhealthy diets high in sugar and fat also play a significant role in increasing your risk of diabetes; 80 per cent of those with Type 2 diabetes are overweight or obese."
In Michael's case there were also mood swings. On top of this, he had a significant family history of type 1 diabetes (where you inject insulin). His father and a couple of uncles developed the auto-immune condition, but only when they were in their sixties. Eventually, of course, he did see a doctor and was diagnosed by a simple blood test.
But, and this was our first piece of misfortune with the healthcare in south-east England where we were living, they thought he had type 2 diabetes and simply put him on pills and a different diet. So wrong, but we didn't know.
I was so relieved I remember bursting into tears, as I'd been certain my partner was on the way out with something like leukaemia. He didn't react well, as he knew something of the implications because of his dad and wasn't happy about the possibility of eventually becoming insulin-dependent.
Life went on; we were both busy but we fairly soon realised that Michael wasn't getting better as he should. This was when I had a real battle on my hands as he was in denial and almost refused to go back to the doctor.
Things were made more complicated because Michael had just started working for a new booksellers in Canterbury and was putting in ridiculous hours planning author events.
The medics had failed to pick up on how ill he was, but I knew. I saw how he became breathless when we went swimming, how very thin he had become (again), and how tired. It was more than worrying and I consulted a friend at church, Hilary, who was a specialist diabetic nurse. I knew if nothing changed that Michael was probably headed for a potentially fatal diabetic coma and so I asked her what to look out for.
Eventually, we got Michael an appointment with Hilary's boss, the diabetic consultant, and he reluctantly agreed to go. I was still worried he'd bunk off and actually phoned his manager to say he had to attend.
How right I was. Michael went to our local hospital and not only didn't come back home that evening, he had to stay in for a week while they stabilized his blood sugar levels and checked his general health. When I saw the consultant the same day, his furious face was a picture. You could tell that he was thinking 'Why on earth didn't I see this man sooner?' Fortunately, Michael's organs, including his heart, had not been affected.
But we had to live with the consequences. Michael regularly injects insulin before meals now (he calls it his rock star gesture), taking frequent blood readings to fine tune the amount he injects. Recently, with the support of his employer Waterstones, he attended a course in carb counting at Belfast City Hospital’s diabetic clinic to improve his understanding of his insulin levels and his condition generally.
I have to say that the healthcare in Belfast at the Clifton Street Surgery and elsewhere has been superb. Michael sees a diabetic nurse regularly, can air any problems he has and has his eyesight and foot health tested.
Diabetes can in extreme cases cause blindness and some sufferers develop such bad foot problems that amputation is the only answer. But diabetes can be controlled and there are regular advances in research which point the way to an easier future involving insulin pumps transplanted under the skin and other innovations.
It's a hopeful picture once you're diagnosed. We do use a diabetic recipe book, when I remember, and try to lead a relatively healthy lifestyle.
Of course, it isn't always plain sailing and Michael has had bad hypos, usually in the middle of the night, when his blood sugar plummets maybe because he has miscalculated his final insulin jab.
Then I have to run downstairs and raid the kitchen larder for a jam sandwich or biscuits which instantly remove the horrid symptoms of a hypo - trembling, sweating and weakness. Scary stuff.
I was given an injection kit to use in case Michael ever went the other way and was in a coma but doubt I would have been able to use it.
The main thing, though, is that I got my husband back.
*****
What is diabetes?
Diabetes is a condition where the amount of glucose in your blood is too high because the body cannot use it properly. This is because your pancreas doesn’t produce any insulin, or not enough insulin, to help glucose enter your body’s cells – or the insulin that is produced does not work properly (known as insulin resistance).
Insulin is the hormone produced by the pancreas that allows glucose to enter the body’s cells, where it is used as fuel for energy so we can work, play and generally live our lives. It is vital for life. Glucose comes from digesting carbohydrate and is also produced by the liver.
If you have diabetes, your body cannot make proper use of this glucose so it builds up in the blood and can’t be used as fuel. It's estimated that there are 3.3 million diabetics in the UK and about 590,000 who are sufferers but don't know it.
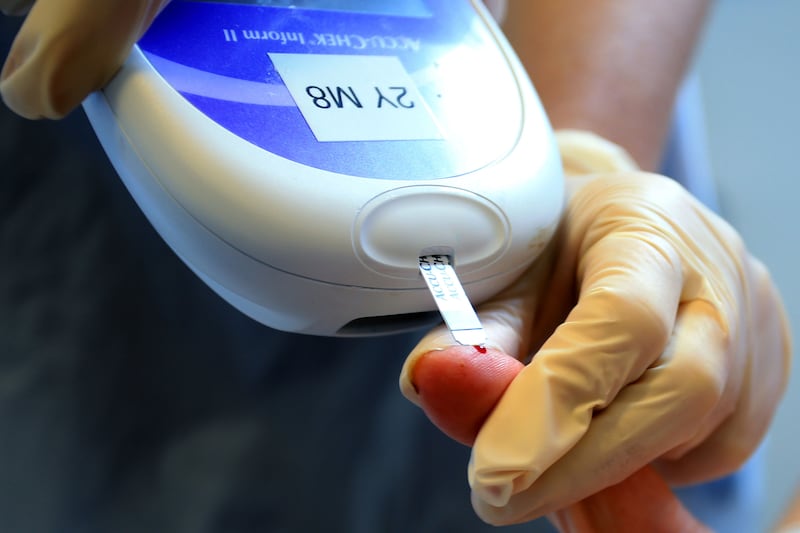
If you experience any of the symptoms listed in the main article, you should make an appointment with your GP as soon as possible. Florence Findlay White of Diabetes UK points out that diagnosis is made through a simple blood glucose measurement.
"People diagnosed with Type 1 diabetes start insulin therapy straight away as they have stopped producing their own insulin and we need it to survive,” she says. "Sometimes patients with Type 2 will also be prescribed medication to enable the body to use the insulin they naturally produce more effectively. As time goes on, the nature of Type 2 diabetes means that more medication may be required to keep the blood glucose at normal levels avoiding the risk of complications such as diabetic eye or kidney disease, heart attack, stroke or amputation."