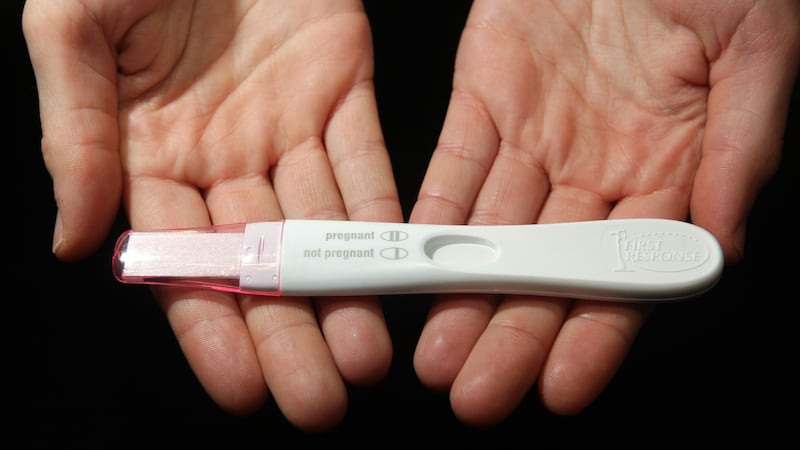
A “wee-stick” test similar to the one used to confirm pregnancy could potentially prevent thousands of ovarian cancer deaths.
Scientists have identified a small protein produced by ovarian tumours that could provide a new way of identifying the disease at early stages.
Work is now under way to see if the biomarker, currently known only as OCP (ovarian cancer protein), can be detected in urine.
Research so far indicates that such a test could lead to a huge improvement in survival rates – possibly from 20% to 90%.
Each year more than 7,000 women in the UK are diagnosed with ovarian cancer and 4,227 die from the disease.
Ovarian cancer is nicknamed the “silent killer” because it so often goes unnoticed until it has progressed to a deadly advanced stage.
Lead researcher Dr Barbara Guinn, from the University of Hull, said: “The majority of diagnoses for ovarian cancer come during stage three, when the cancer has spread to other areas of the body, which has a direct impact on the chances of patients surviving.
“A stage three diagnosis can mean survival rates as low as 20%, but with early detection, that can be increased dramatically to around 90%.”
Although the research is still at an early stage, the hope is that it will lead to screening for early stage ovarian cancer within two or three years.
Speaking at the British Science Festival at the University of Hull, Dr Guinn said: “Our biggest hope is that we find this protein in urine and it will provide a screening method for patients who go into a well-woman clinic, probably to have their breast check and do a urine test, usually for glucose.
“At the same time hopefully we’d have a test for ovarian cancer as well.”
The work done so far indicated that it was “reasonably likely” that OCP would show up in urine, she said.
Dr Guinn envisaged a test similar to the familiar one used to show if a woman is pregnant.
It would have a line indicating a negative result and another line showing the possible presence of ovarian cancer.
The research by her University of Hull team, which has not yet been published, involved looking for the protein in tissue samples.
OCP was found in 18% of stage one tumour samples, 36% of stage two samples, and 17% of stage three samples. However the laboratory tests were designed to require a high detection score before being classified as “positive”.
The tests seemed to suggest that levels of the protein actually reduced as the cancer progressed from stage two to stage three, said Dr Guinn.
She added that the protein appeared to be involved in the development of ovarian tumours, raising the possibility of a therapeutic target as well as a diagnostic tool.
“If you could knock out that protein and remove it you could potentially stop the tumour growing,” said Dr Guinn.
The protein was found in all types of ovarian cancer, but did not appear to be detectable in blood, she said.
Annwen Jones, chief executive of the charity Target Ovarian Cancer, Annwen Jones, said: “Early detection of ovarian cancer is the holy grail. Research into new biomarkers shows extreme promise and we look forward to a future where more women are diagnosed at the earliest possible stage.”